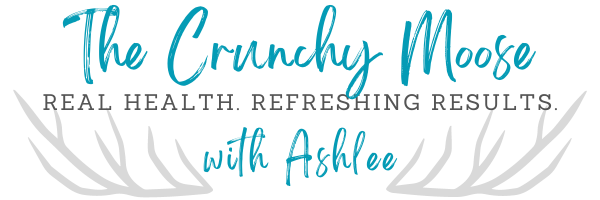It's the big day! We're picking up our daughter from NICU! She's coming home after 3 weeks in the hospital!
Picture it. It's July in Texas. The temperature outside is 98o. It's about 4:00 pm and rush hour traffic is starting to pile up.
We pull the car seat straps as small as they could go and fumble around to get our hands in there to buckle up our little 4 pound bundle of joy, Mabel Rose.

We hop on the highway and within a couple minutes we are at a complete stop. I'm in the backseat with Mabel. My husband, Ryan, hops out of the car to talk to other drivers to see what's happening.
Ryan tells me that there's a burning banana truck. I tell him that he's in a bad game of telephone and definitely heard wrong.
Turns out, we're about 20 cars behind a burning 18-wheeler full of bananas. Traffic was backed up from 4:30 pm until 1:00 am the next morning.
 |  |  |
Pictures from a news site | ||
It took us 4 hours to drive the 14 miles home.
Cars were running out of gas. It was hot and we have a 4 pound baby straight outta NICU. I'm nursing my first baby (my older son is adopted and bottle fed) and trying to figure that out in the back seat of a hot car.
My best parenting decision ever was to not take my almost 3 year old very active toddler son with us to pick up Mabel! Mabel was fine for 4 hours in the car. Morrison would not have been.
How Did We Get Here?
How did we get stuck behind a burning banana truck? Let's back up and look at my pregnancy.
I had a beautiful and easy pregnancy with no complications -- something the doctors told me was never possible due to my back surgeries (I have a fusion with hardware in my spine. Read more about that here.)
I loved being pregnant. I craved clementine oranges and ate pounds and pounds of them. I was never nauseous and only got sick once (keep reading for why). What I lacked in nausea, I made up in exhaustion. I was extremely tired and had trouble keeping up with my toddler son and some days even getting out of bed.

My Birth Plan
I had a birth plan. But Mabel had a different plan.
I chose a midwife that had privileges at a birth center and at a hospital. My plan was to be at the birth center but wanted the hospital option in case I had complications with the fusion in my back.)
The only time I got nauseous during my pregnancy was at 22 weeks. I had my first ultrasound. It was a standard ultrasound-- topical on my abdomen.
I went home and was extremely sick for 24 hours.
I had a horrible reaction to the ultrasound.
My assumption is that the hardware in my spine reacted to the frequencies from the ultrasound. I spoke to my midwife and opted out of ultrasounds for the remainder of my pregnancy.
***IMPORTANT NOTE: I am not against ultrasounds during pregnancy. That is not why I am telling my story and I'm not even presenting that as a debate topic. Ultrasounds are extremely useful and amazing and have been very beneficial in many pregnancies. I had a bad reaction to them. This is a *me* problem and not a blanket statement about ultrasounds.
7 Weeks Early
At 32 weeks and 6 days, I had a checkup with my midwife. Since I was doing a birth center birth and had a history of back problems, she wanted to do a quick ultrasound just to make sure everything was good.
The ultrasound showed that all of her vitals were great....except her head. It showed that her head was at the 3rd percentile.
I was sent to a specialist that did extensive scans. Those scans also showed her head was extremely small.
I was sent home for bed rest.
I had another bad reaction to the ultrasound. Mabel was born the next day at 33 weeks -- 7 weeks early.
I had 2 ultrasounds during my pregnancy. After the 1st one, I was sick for 24 hours. After the 2nd one, I went into early labor that night.
I woke up in the middle of the night and my water had broken in my sleep.
We went to the hospital that my midwife had privileges to. The hospital had closed their maternity ward the week before and we had no idea. We were transferred to a hospital in the next city.
Mabel was born at 1:12 pm, 4 pounds 3 ounces, 17".
Her head was perfect and the ultrasounds were wrong.
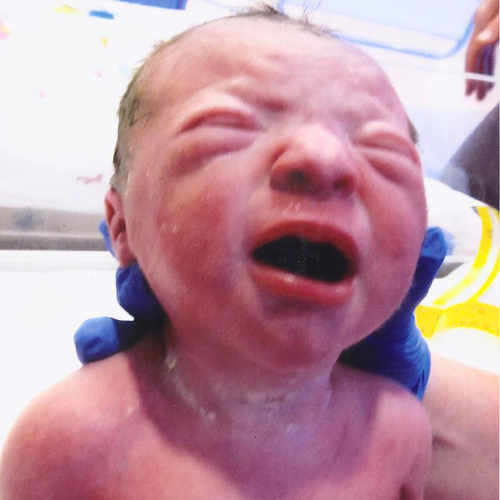
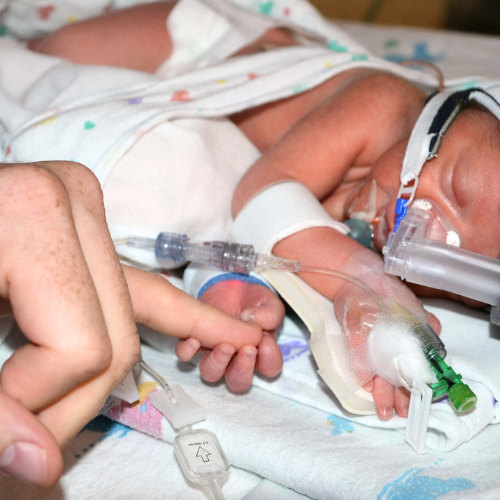
Other than being small, she was healthy and happy! She was in NICU for 3 weeks.
 |  |  |
 |  |  |
Expectations vs Reality
I had Pinterest worthy expectations and plans. The reality was very different.
- I planned on finishing my 6 week birth class. I made it to 2 classes. During labor, the nurse said "time to do your breathing" and I said while pushing "that's next week's class!"
- I planned on taking professional maternity pictures. I bought the outfits and paid the photographer. The photographer shifted and did family pictures for us. And I posed with my maternity outfits with Mabel and Ryan took our picture.
 |  |
- I planned on giving birth at a birth center with my midwife.
- In reality, I gave birth at a hospital I had never been to with doctors I had never met.
- I planned on being able to move around, eat a snack when I needed, and follow my body's cues during labor. And definitely not lay on my back with added pressure on my fusion.
- In reality, I was in a hospital where they made me lay on my back, putting pressure on my fusion. I was rushed to the hospital early in the morning, I had not eaten since the night before and they did not let me eat until after delivery.
- I planned on encapsulating my placenta. I had placenta recipes ready!
- The hospital did not allow it.
- I planned on Mabel being born in the city my husband was born in, where we met, and where we had lived for over a decade.
- We were transferred to a neighboring city and she was born there.
- I planned on skin-to-skin immediately while she took her first breaths.
- The nurses rushed her to NICU when she was born.
- I planned on nursing from the get-go.
- I pumped and pumped and it took a few days for my milk to come in. But once my milk came in, she nursed no problem and I was able to provide bottles for the nurses when I wasn't there.
- I planned on a drug free, natural birth.
- I had a drug free, natural birth!
If I had to have a NICU situation, this was the best NICU situation ever! Mabel was very healthy. I was able to hold her, skin-to-skin whenever I was there. She was able to nurse as soon as my milk came in. The nurses were fantastic.
Back to the Banana Truck
We were able to pick up Mabel at exactly 3 weeks on July 24, 2015. That's the day the banana truck caught on fire.
Her birth didn't go as planned. Our ride home didn't go as planned. But I sure do have a great story to tell!
Mabel's older brother is adopted. Read his adoption story here!
Pin this article to save it for later!
Also check out:
 |  |  |
 |  |  |